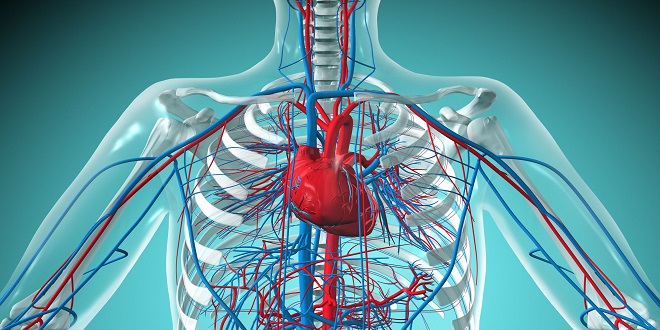
The Vascular System
ARTERIES
Arteries carry blood from the heart to capillaries; smaller arteries are called arterioles. If we look at an artery in cross-section, we find three layers (or tunics) of tissues, each with different functions. The innermost layer, the tunica intima, is the only part of a vessel that is in contact with blood. It is made of simple squamous epithelium called endothelium. This lining is the same type of tissue that forms the endocardium, the lining of the chambers of the heart. As you might guess, its function is also the same: Its extreme smoothness prevents abnormal blood clotting. The endothelium of vessels, however, also produces nitric oxide (NO), which is a vasodilator. The tunica media, or middle layer, is made of smooth muscle and elastic connective tissue.
VEINS
Veins carry blood from capillaries back to the heart; the smaller veins are called venues. The same three tissue layers are present in veins as in the walls of arteries, but there are some differences when compared to the arterial layers. The inner layer of veins is smooth endothelium, but at intervals this lining is folded to form valves. Valves prevent backflow of blood and are most numerous in veins of the legs, where blood must often return to the heart against the force of gravity.
The middle layer of veins is a thin layer of smooth muscle. It is thin because veins do not regulate blood pressure and blood flow into capillaries as arteries do. Veins can constrict extensively, however, and this function becomes very important in certain situations such as severe hemorrhage. The outer layer of veins is also thin; not as much fibrous connective tissue is necessary because blood pressure in veins is very low.
EXCHANGES IN CAPILLARIES
Capillaries are the sites of exchanges of materials between the blood and the tissue fluid surrounding cells. Some of these substances move from the blood to tissue fluid, and others move from tissue fluid to the blood. The processes by which these substances are exchanged are illustrated.
Gases move by diffusion, that is, from their area of greater concentration to their area of lesser concentration. Oxygen, therefore, diffuses from the blood in systemic capillaries to the tissue fluid, and carbon dioxide diffuses from tissue fluid to the blood to be brought to the lungs and exhaled.
PATHWAYS OF CIRCULATION
The two major pathways of circulation are pulmonary and systemic. Pulmonary circulation begins at the right ventricle, and systemic circulation begins at the left ventricle. Hepatic portal circulation is a special segment of systemic circulation that will be covered separately. Fetal circulation involves pathways that are present only before birth and will also be discussed separately.
PULMONARY CIRCULATION
The right ventricle pumps blood into the pulmonary artery (or trunk), which divides into the right and left pulmonary arteries, one going to each lung. Within the lungs each artery branches extensively into smaller arteries and arterioles, then to capillaries. The pulmonary capillaries surround the alveoli of the lungs; it is here that exchanges of oxygen and carbon dioxide take place. The capillaries unite to form venues, which merge into veins, and finally into the two pulmonary veins from each lung that return blood to the left atrium. This oxygenated blood will then travel through the systemic circulation. (Notice that the pulmonary veins contain oxygenated blood; these are the only veins that carry blood with a high oxygen content. The blood in systemic veins has a low oxygen content; it is systemic arteries that carry oxygenated blood.)
SYSTEMIC CIRCULATION
The left ventricle pumps blood into the aorta, the largest artery of the body. We will return to the aorta and its branches in a moment, but first we will summarize the rest of systemic circulation. The branches of the aorta take blood into arterioles and capillary networks throughout the body. Capillaries merge to form venues and veins.
HEPATIC PORTAL CIRCULATION
Hepatic portal circulation is a subdivision of systemic circulation in which blood from the abdominal digestive organs and spleen circulates through the liver before returning to the heart. Blood from the capillaries of the stomach, small intestine, colon, pancreas, and spleen flows into two large veins, the superior mesenteric vein and the splenic vein, which unite to form the portal vein. The portal vein takes blood into the liver, where it branches extensively and empties blood into the sinusoids, the capillaries of the liver. From the sinusoids, blood flows into hepatic veins, to the inferior vena cava and back to the right atrium. Notice that in this pathway there are two sets of capillaries, and keep in mind that it is in capillaries that exchanges take place. Let us use some specific examples to show the purpose and importance of portal circulation.
VELOCITY OF BLOOD FLOW
The velocity, or speed, with which blood flows differs in the various parts of the vascular system. Recall that it is in capillary networks that exchanges of nutrients, wastes, and gases take place between the blood and tissue fluid. The slow rate of blood flow in capillaries permits sufficient time for these essential exchanges. Think of a train slowing down (not actually stopping) at stations to allow people to jump on and off, then speeding up again to get to the next station. The capillaries are the “stations” of the vascular system.
BLOOD PRESSURE
Blood pressure is the force the blood exerts against the walls of the blood vessels. Filtration in capillaries depends upon blood pressure; filtration brings nutrients to tissues, and as you will see in Chapter 18, is the first step in the formation of urine. Blood pressure is one of the “vital signs” often measured, and indeed a normal blood pressure is essential to life. The pumping of the ventricles creates blood pressure, which is measured in mmHg (millimeters of mercury). When a systemic blood pressure reading is taken, two numbers are obtained: systolic and diastolic, as in 110/70 mmHg. Systolic pressure is always the higher of the two and represents the blood pressure when the left ventricle is contracting. The lower number is the diastolic pressure, when the left ventricle is relaxed and does not exert force. Diastolic pressure is maintained by the arteries and arterioles and is discussed in a later section.
REGULATION OF BLOOD PRESSURE
The mechanisms that regulate systemic blood pressure may be divided into two types: intrinsic mechanisms and nervous mechanisms. The nervous mechanisms involve the nervous system, and the intrinsic mechanisms do not require nerve impulses.
AGING AND THE VASCULAR SYSTEM
It is believed that the aging of blood vessels, especially arteries, begins in childhood, although the effects are not apparent for decades. The cholesterol deposits of atherosclerosis are to be expected with advancing age, with the most serious consequences in the coronary arteries. A certain degree of arteriosclerosis is to be expected, and average resting blood pressure may increase, which further damages arterial walls. Consequences include stroke and left-sided heart failure.
The veins also deteriorate with age; their thin walls weaken and stretch, making their valves incompetent. This is most likely to occur in the veins of the legs; their walls are subject to great pressure as blood is returned to the heart against the force of gravity. Varicose veins and phlebitis are more likely to occur among elderly people.
SUMMARY
Although the vascular system does form passageways for the blood, you can readily see that the blood vessels are not simply pipes through which the blood flows. The vessels are not passive tubes, but rather active contributors to homeostasis. The arteries and veins help maintain blood pressure, and the capillaries provide sites for the exchanges of materials between the blood and the tissues. Some very important sites of exchange are discussed in the following chapters: the lungs, the digestive tract, and the kidneys.